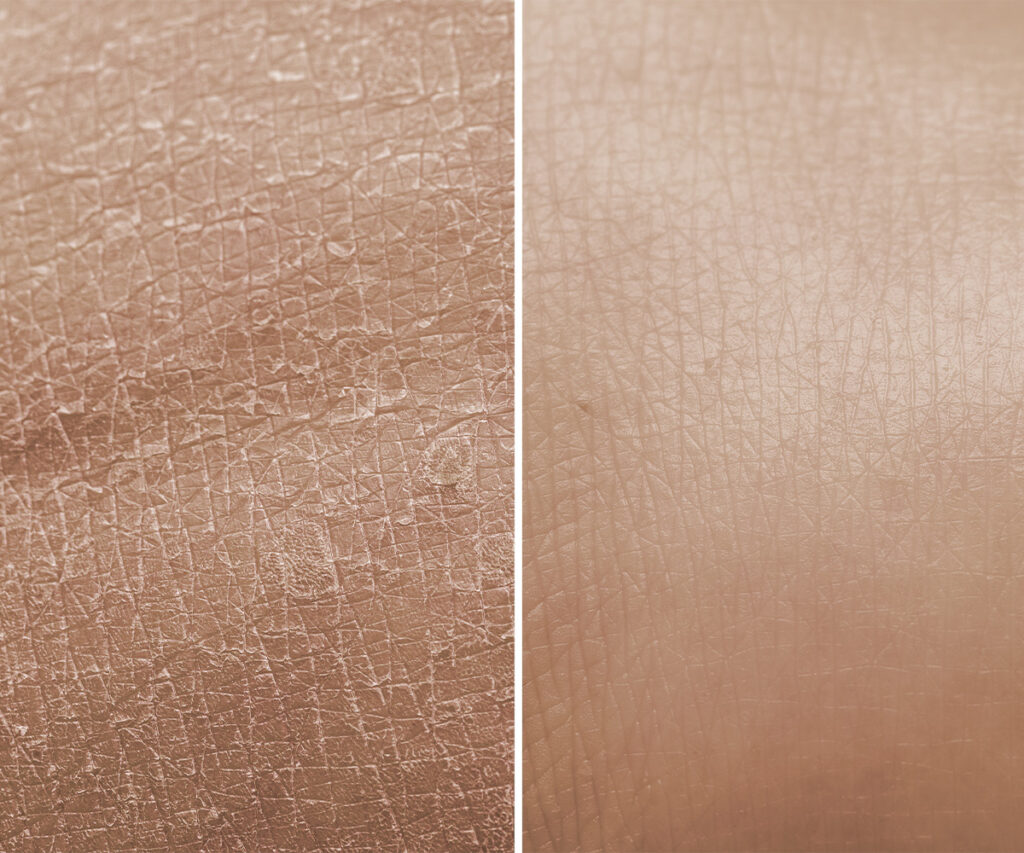
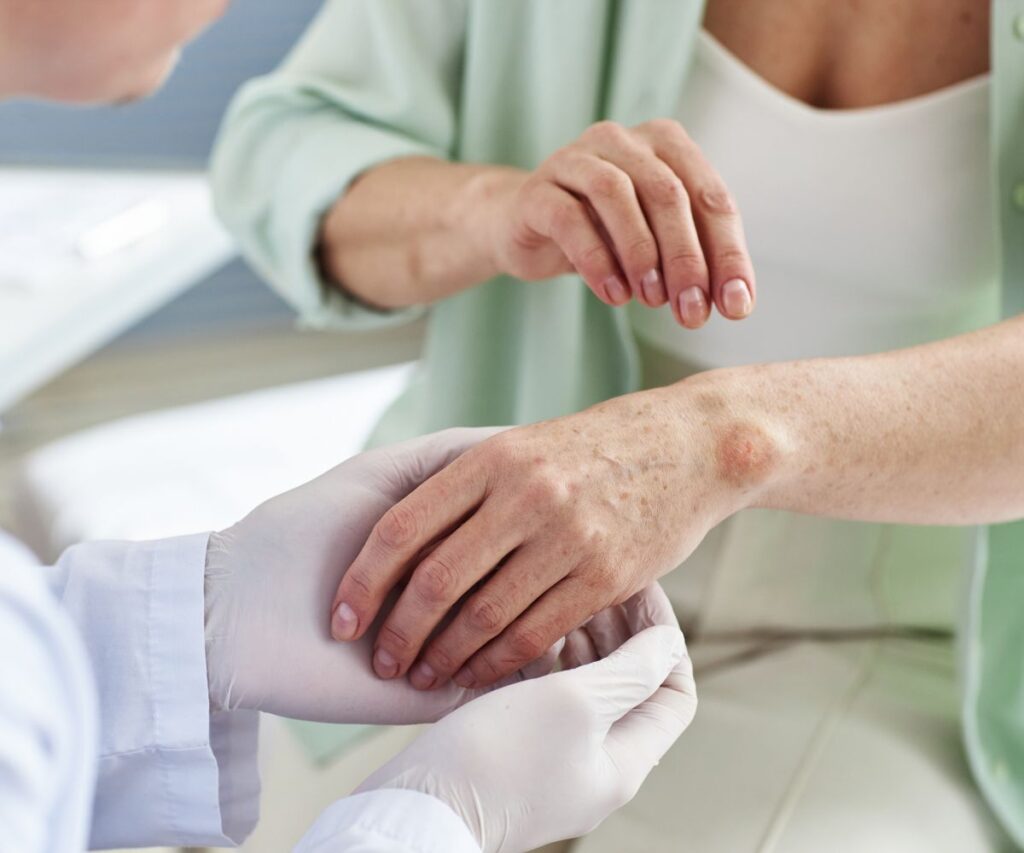
During the course of chemotherapy, the skin can become particularly vulnerable. It is essential to pay attention to sunscreen to prevent damage and irritation, not only during treatment, but also during the recovery period.
1. Skin and Chemotherapy
Chemotherapy can cause significant side effects on the skin, including:
- Dryness: Skin may lose moisture and become rough.
- Increased sensitivity: Therapies can make the skin more prone to sunburn and irritation.
- Risk of sunburn: Treatments can increase UV sensitivity, making sunscreen even more crucial.
2. Why Sun Protection is Essential
- Sunburn Prevention.: The use of a broad-spectrum sunscreen helps protect the skin from damage caused by UVA and UVB rays.
- Reducing the Risk of Skin Cancer.: Sun protection reduces the risk of developing forms of skin cancer, which is especially important for those who have already faced a cancerous disease.
- Maintaining Skin Health: Using sunscreen products helps maintain skin elasticity and health, minimizing signs of premature aging.
3. How to Choose Sunscreen
When choosing a sunscreen, consider:
- Sun Protection Factor (SPF).: Opt for an SPF of 30 or higher.
- Water Resistance.: Choose a water-resistant product, especially if you plan to sweat or swim.
- Gentle ingredients: Prefer formulas without fragrances and additives that irritate sensitive skin.
4. Application and Reapplication
- Generous Application: Apply an appropriate amount of sunscreen to all exposed areas of the skin at least 30 minutes before going outside.
- Reapplication: Reapply every two hours, or more frequently if you are in water or sweating.
5. Sun Protection After Chemotherapy
Even after completing chemotherapy, the skin remains vulnerable. Continuing to use sunscreen daily is critical to:
- Supporting Healing: Help the skin recover and protect any treated or damaged areas.
- Prevent Future Damage.: Continue the sunscreen routine to reduce the risk of long-term complications.
Conclusion
Sun protection is an essential element for those going through chemotherapy and the recovery period. Adopting a sunscreen routine can make a big difference in your skin health and overall well-being. Be sure to always consult your doctor or dermatologist for personalized advice.