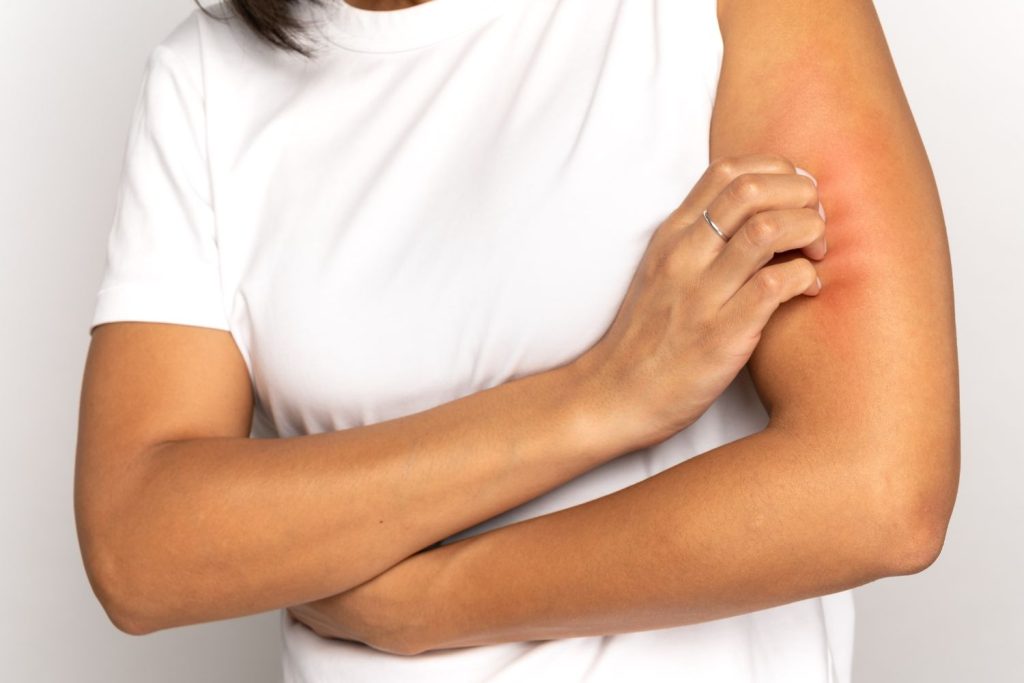
Both external and internal factors can alter the defense mechanisms and cause severe skin dehydration and flaking of the facial skin.
That is why skin care is critical during treatment. Side effects can be debilitating and can impair the patient’s quality of life.
What is facial skin desquamation
Skin desquamation refers to the loss of the most superficial layer of the epidermis, known as the stratum corneum. Scaling causes an accumulation on the skin of scales, which is typical of dry, dehydrated skin and sometimes also results in redness, burning, and itching.
Skin desquamation can have different characteristics and coloration:
- fine and read;
- In the shape of fish scales;
- oily and greasy;
- grayish-white;
- yellow.
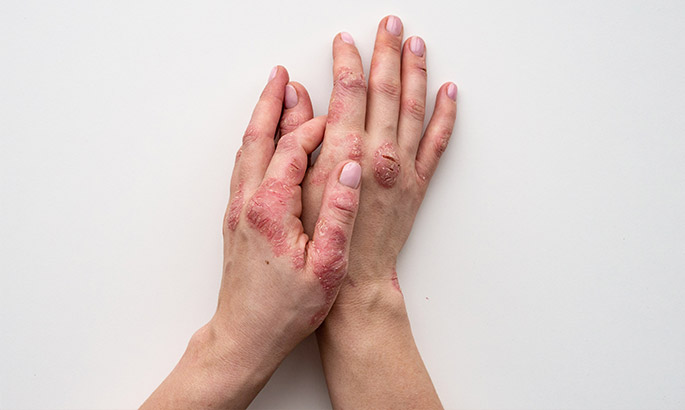
In addition, skin flaking, besides causing discomfort and itching, can lead to other disorders, such as contact dermatitis (inflammation of the skin caused by direct contact with irritants) and infection.
Skin desquamation, affects various areas of the body, but the areas where it is most noticeable and also most common is undoubtedly the face.
The face, is one of the parts of our body that has a thinner epidermis and stratum corneum (as well as being more exposed to the elements). For these very reasons it is more common to occur in this area of the body. Initially it manifests as tightness and roughness, but if left untreated the situation can worsen and the skin can become very tight and flaky, causing much itching and discomfort.
The causes of facial skin flaking
The causes of facial skin peeling can be many: in case of sunburn, burn, or it can occur as a result of some dermatological diseases, such as eczema, but also due to cancer therapies. To alleviate the problem you can use our moisturizing facial cleanser, a gentle emulsion formulated to cleanse and moisturize the skin of the face and neck.
Why does the skin flake?
There is desquamation of the skin; when lipids are present in minimal amounts, the skin stops acting as a barrier and therefore “water loss” is more likely to occur. This results in dry and flaky skin, looking less radiant and sometimes even rough.